Whether you choose traditional childbirth or a natural childbirth approach, you may want or need medical intervention. The two most common medical interventions during labor and vaginal delivery are managing pain and inducing labor.
Some women plan to have a more natural childbirth experience, but may want or need pain medication during labor. If your labor is longer or more difficult than expected – or you simply change your mind – there’s no shame in deciding that medication is right for you. However, there may be a “point of no return,” when it’s too late to start certain types of pain medications for a vaginal delivery. If you have questions about pain medication, ask your health care provider.
Pain management
If you would like to manage your pain medically, talk with your health care provider about your options. The two of you can discuss the risks and benefits of different types of pain medications, including what is the safest and most effective option for you and your baby. The best choice for you will be determined by:
- your preference
- your health
- the health of your baby
- your health care provider’s recommendations
There are two main types of pain medications given during labor and delivery. Those are:
- Analgesics, which are medications, such as meperidine, that are meant to relive pain. Small amounts are usually safe during labor. They are used often and carry very few risks of complications. However, if they are given in large or repeated doses, they can cause respiratory depression (slowing of the breathing center in the brain) in both mothers and babies.
- Anesthesia is a medication that causes loss of sensation. There are a few different types of anesthesia used during labor and delivery:
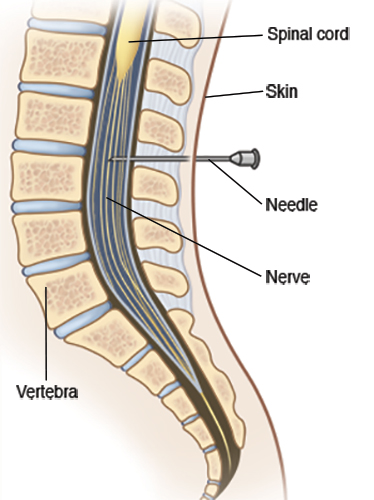
- Epidural anesthesia (also called an epidural block) involves giving medications through a thin catheter that has been inserted into the space that surrounds the spinal cord in the lower back. Infusions of medications may be increased or stopped as needed. This type of anesthesia is used during labor and for vaginal and cesarean deliveries. The most common complication of epidural anesthesia is low blood pressure in the mother. Because of this, most woman need to have an intravenous infusion of fluids before epidural anesthesia is given. One risk of epidural anesthesia is a postpartum headache. It may develop if the epidural needle enters the spinal canal rather than staying in the space around the canal. If you choose to or need to have anesthesia, the anesthesiologist will discuss with you the risks, benefits and alternatives to the various methods of pain relief.
- Epidural analgesia is is sometimes called a "walking" epidural because the medication infused through the epidural is an analgesic, which relieves pain but does not numb the body and allows for movement, unlike epidural anesthesia. You cannot, however, actually walk around after receiving the medication. Combinations of medications may be used in the epidural. For example,part analgesic, part anesthetic. The most common complication of epidural analgesia is low blood pressure in the mother. This type of anesthesia is used during labor and for vaginal deliveries. You may also develop a postpartum headache from epidural analgesia.
- Local block is anesthesia that is injected in the perineal area (the area between the vagina and rectum) that numbs the area to make repair of a tear or episiotomy much easier for women to tolerate.
- Pudendal block is a type of local anesthesia that is injected into the vaginal area to cause complete numbness in the vaginal area without affecting the contractions of the uterus. If a woman has this type of block, she can remain active in pushing her baby through the birth canal. It is used for vaginal deliveries
- Spinal anesthesia involves injecting a single dose of the anesthetic agent directly into the spinal fluid. Spinal anesthesia acts very quickly, and it causes complete loss of sensation and loss of movement of the lower body. This type of anesthesia is often used for cesarean deliveries.
- General anesthesia involves giving an anesthetic agent that causes the woman to go to sleep. This type of anesthesia may be used in emergency cesarean deliveries.
Inducing Labor
In some cases, labor has to be "induced," which is a process of stimulating labor to begin. The reasons for induction vary. Labor induction is not done before 39 weeks of pregnancy unless there is a problem. Some common reasons for induction include:
- the mother and/or fetus are at risk
- the pregnancy has continued too far past the due date
- the mother has preeclampsia, eclampsia or chronic high blood pressure
- the fetus has been diagnosed with poor growth
Some common techniques of induction include:
- misoprostol pills that are either taken orally or placed vaginally to ripen the cervix for delivery
- administering an intravenous infusion of oxytocin (a hormone produced by the pituitary gland that stimulates contractions) or administering a similar drug
- rupturing the amniotic sac
What is Oxytocin?
Oxytocin (ox-e-TOE-sin) is a synthetic form of a natural hormone. It works by causing the uterus to contract. It is used to increase the strength and/or frequency of contractions of the uterus. Oxytocin can be used during childbirth to move a women into labor or after childbirth to control bleeding. This medicine must be infused into a vein. It is given by a health care provider in a hospital or clinic setting.
Although rare, there are some potential side effects of oxytocin. If you experience any side effects let your health care provider know as soon as possible.